Waking up with a throbbing pain that radiates through your teeth, up your jaw, and into your ear is an overwhelming experience. It’s hard to pinpoint exactly where the pain is starting, which often leaves patients wondering: Should I call a doctor for an ear infection, or do I need a dentist?
In most cases, when the pain is isolated to one side of your face and involves the jawline, the root cause is dental. Here is a clinical breakdown of why this happens, what might be causing your discomfort, and when you need to seek immediate care.
Why Are My Tooth, Jaw, and Ear Connected?
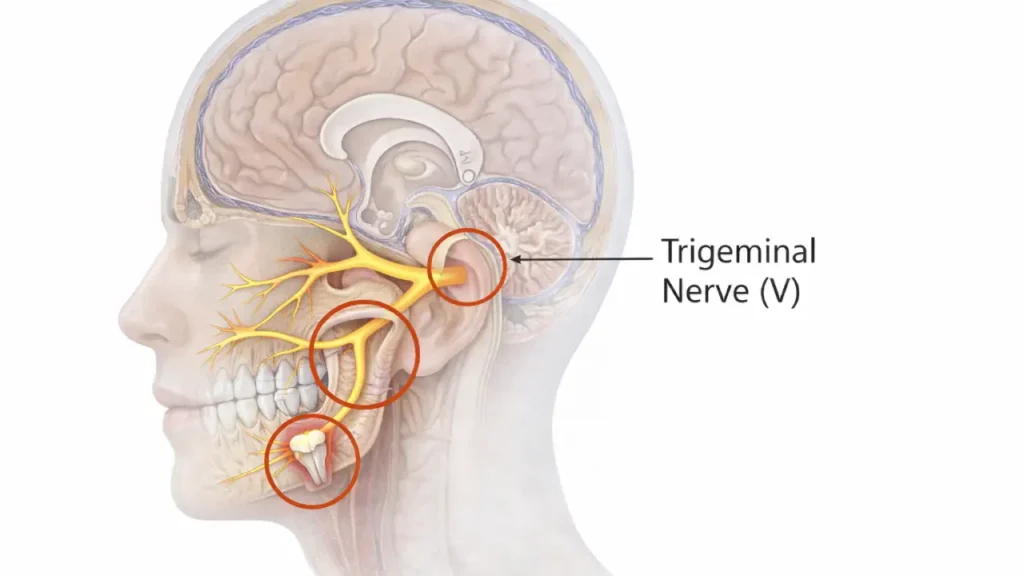
To understand your pain, you have to look at the anatomy of your face. Your jaw, teeth, and gums are all wired to the brain via the trigeminal nerve. This is the largest sensory nerve in your head.
Because the branches that serve your upper and lower jaw run extremely close to the structures of your inner ear, a strong pain signal from a single tooth can easily cross over. Your brain misinterprets the origin of the signal, causing you to feel a severe earache when the actual problem is a dying tooth nerve. In dentistry, we call this “referred pain.”
Can a Tooth Infection Cause Jaw and Ear Pain?
Yes, and this is one of the most common reasons for this specific type of pain. When tooth decay is left untreated, bacteria bypass the hard enamel and reach the inside of the tooth, eventually traveling down the root into the jawbone.
This creates a dental abscess, a localized pocket of pus and severe inflammation. Because the infection is trapped beneath the gumline and inside the bone, the pressure has nowhere to go. This extreme pressure causes a severe, throbbing ache that radiates outward.
Signs you have an abscess include:
-
Pain that worsens when you chew or tap on the tooth.
-
A foul taste or odor in your mouth.
-
Swollen, red gums around a specific tooth.
Could It Be a Deep Root Infection? (Signs You Might Need a Root Canal)
Before a full abscess forms, the soft tissue inside your tooth (the pulp) becomes inflamed. When bacteria infect the pulp, the nerve begins to die. The resulting pain is typically described as a sharp, shooting, or intense throbbing that keeps you awake at night and travels straight up your jaw to your ear.
You cannot diagnose a root infection by just looking in the mirror. At Vela Dental, we use advanced digital imaging to look beneath the gumline and evaluate the exact health of your tooth roots.
If the nerve is infected, the solution is Root Canal Therapy. Many patients fear root canals due to outdated myths, but the reality is that a modern root canal does not cause pain, it is the exact procedure designed to eliminate the severe pain you are feeling right now by removing the infected tissue.
Is TMJ to Blame for My Earache and Jaw Pain?
If your pain feels more like a constant, dull ache rather than a sharp throb, you might be dealing with a Temporomandibular Joint (TMJ) disorder.
Place your fingers just in front of your ears and open your mouth. That hinge you feel is the TMJ. Because the joint is situated millimeters away from your ear canal, inflammation here is frequently mistaken for an ear infection.
TMJ pain is often triggered by bruxism (unconsciously clenching or grinding your teeth while you sleep). If you wake up with a stiff jaw, tension headaches, and earaches, grinding is the likely culprit. A custom-fitted Night Guard can protect your teeth and relieve the tension on the joint.
Can Impacted Wisdom Teeth Make My Ear Hurt?
If you are between the ages of 17 and 25, or if you still have your third molars, impacted wisdom teeth are a primary suspect for jaw and ear pain.
When a wisdom tooth doesn’t have enough room to erupt properly, it can get stuck against the adjacent molar or partially break through the gums. This creates a flap of tissue that traps food and bacteria, leading to a painful localized infection called pericoronitis. The swelling from the back of the mouth easily spreads to the jaw muscles and radiates up to the ear.
How Can I Relieve Jaw and Ear Pain at Home?
While you wait for your dental appointment, you can manage the discomfort with a few safe at-home methods:
-
Anti-inflammatories: Over-the-counter ibuprofen is generally more effective for dental pain than acetaminophen because it reduces tissue inflammation.
-
Cold and Warm Compresses: Use an ice pack wrapped in a towel for 15 minutes to numb sharp pain and reduce swelling. If the pain is muscular (like TMJ), a warm, damp towel can help relax the jaw.
-
Keep your head elevated: Lying flat increases blood pressure in your head, which makes a throbbing toothache worse. Sleep with your head propped up on extra pillows.
Clinical Warning: Never place a crushed aspirin directly against your gums or the painful tooth. This is an old myth that will result in a severe chemical burn on your tissue.
Is Jaw and Ear Pain a Dental Emergency? (When to See a Dentist ASAP)
Certain symptoms mean the infection is spreading and requires immediate intervention. You need to see an Emergency Dentist immediately if your pain is accompanied by:
-
Visible swelling on your face, cheek, or under your eye.
-
A fever.
-
Difficulty swallowing or breathing.
-
Inability to fully open your mouth.
Tooth and jaw pain that disrupts your life is not something you have to tough out. If you are experiencing severe discomfort, our team at Vela Dental is here to help. Call our Corpus Christi office immediately at (361) 884-6663 so we can evaluate your symptoms, get you out of pain, and protect your oral health.